Because lean methodologies are designed to eliminate waste and improve efficiency, they are particularly effective in streamlining processes. One key aspect of lean methodologies is the identification of value-added activities, which are those tasks that directly contribute to value of the product or service, versus non-value-added services.
By Lisa Mead, RN, MS, CPHQ, CHPC
Radiology practices play a crucial role in health care, providing medical imaging services that aid in diagnosing and treating a wide range of medical conditions. When radiology departments experience staffing shortages, repercussions are felt throughout the enterprise with a significant impact on patient care and overall efficiency. Quality methods can help radiology practices improve efficiency during staffing shortages and ensure that patients receive timely and accurate diagnoses and treatment.
Quality methods can help radiology practices improve efficiency during staffing shortages and ensure that patients receive timely and accurate diagnoses and treatment.
The benefits of using quality methods in radiology are numerous and have the potential to significantly impact the overall quality of care provided to patients. Some of the key benefits of using quality methods in radiology include:
Improved patient outcomes. Improved accuracy and timeliness of diagnoses lead to better patient outcomes, including earlier detection of diseases, more effective treatment plans, and improved overall health outcomes for patients.
Increased efficiency. Quality methods can help radiology practices streamline their workflows and reduce the amount of time required to perform tasks. This can help practices work more efficiently, even during staffing shortages, and ensure that patients receive timely care.
Reduced errors. By streamlining workflows, using technology, and cross-training staff, radiology practices can reduce the likelihood of errors and ensure that patients receive accurate diagnoses and treatment.
Increased patient satisfaction rates. Patients are more likely to be satisfied with their care when they receive prompt and accurate diagnoses, which can lead to improved patient retention and word-of-mouth referrals.
Reduced costs. By improving efficiency and reducing error, radiology practices can potentially save money on staffing, equipment, and other expenses, while also improving the quality of patient care.
Process Improvement
A quality method that is particularly helpful in improving efficiency during staffing shortages is process improvement, which entails analyzing existing processes to identify areas that can be improved. Through process improvement techniques, radiology workflows can be streamlined, time required to perform tasks reduced, the likelihood of errors decreased, and the bandwidth of existing personnel increased.
Because lean methodologies are designed to eliminate waste and improve efficiency, they are particularly effective in streamlining processes. One key aspect of lean methodologies is the identification of value-added activities, which are those tasks that directly contribute to value of the product or service, versus non-value-added services. Eliminating non-value-added activities enable radiology groups to reduce the amount of time required to complete task, thereby freeing up staff time to focus on higher-priority activities.
Lean in health care is defined by an organization’s cultural commitment to applying the scientific method to designing, performing, and continuously improving the work delivered by teams of people leading to measurably better value for patients and other stakeholders.
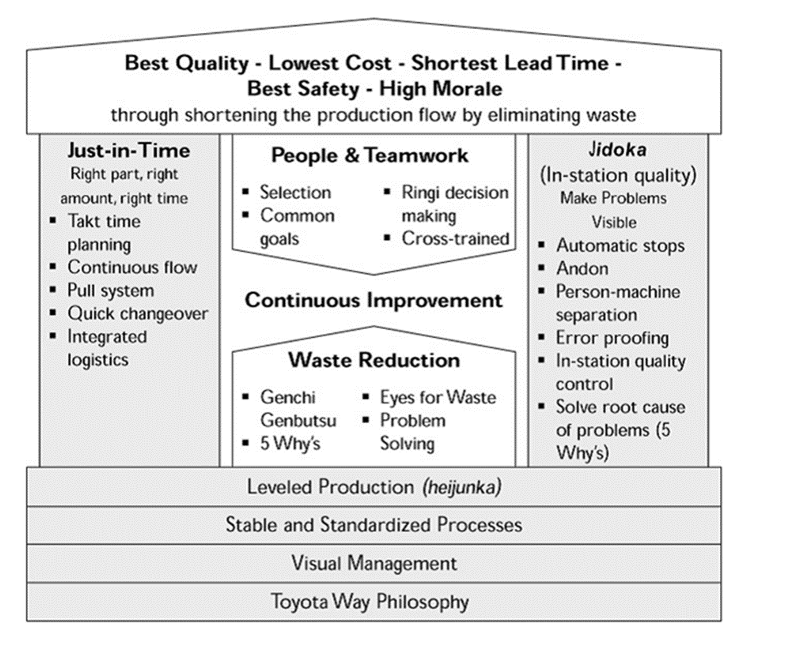
Lean Manufacturing Principles Do Apply
Lean methodologies originated in manufacturing, but the same principles apply to health care that apply to manufacturing, as visualized in this diagram of the Toyota Production System.
Radiology practices that are interested in taking this journey can begin by implementing the following eight steps:
Step 1. Identify a lean operation leader.
Step 2. Education of organization executives and leaders.
Step 3. Design the organization lean system.
Step 4. Introduce the entire staff to the new lean system.
Step 5. Implement basic training and basic first steps.
Step 6. Form lean implementation teams.
Step 7. Identify areas of improvement with value stream map.
Step 8. Start executing Kaizens – continuously improve practices.
Improving Radiologist Productivity: A Case Study
For example, if a radiology practice wishes to improve radiologist productivity, it would begin by establishing goals. Those goals may include the following:
• Increase radiologist productivity (wRVU) per shift from 60 to 70 wRVU/shift.
• Decrease variation in productivity between radiologists in a shift.
The practice would then determine the approach that works best in its particular practice setting. For example:
• Phased approach; one clinical section at a time
• Focus on low- and medium-hanging fruit
• Multi-faceted approach to include process-based approach (Lean); data-based approach (Data Analysis, Statistics); input from radiologists and staff
• Observations and recommendations are presented to the section and the Board at the appropriate level of implementation: (practice-wide; section-wide; individual if applicable)
• Implementation and monitoring
Develop Process Map to Identify Waste
Once the practice has established the goals, the next step is to develop a process map that will help the group to identify wastes. In the example mapped below, multiple wastes are identified.
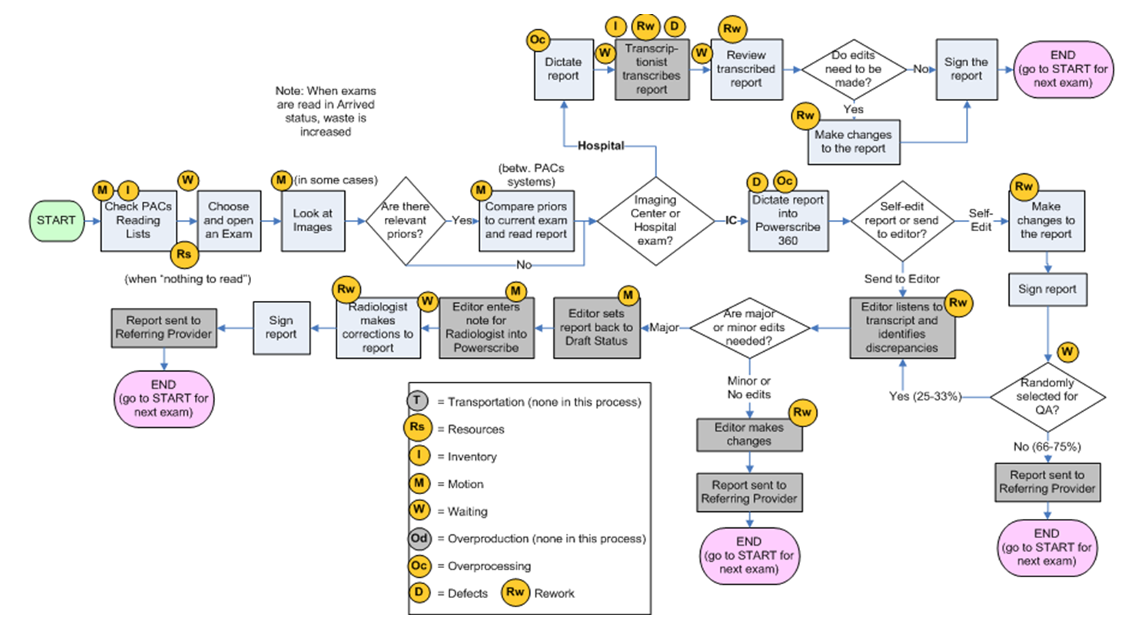
Blue—radiologist activity; Gray—transcriptionists and others
Key Improvements
Using the Process Map visualized above that identified waste, this practice was able to implement key improvements in four areas that enabled the practice to improve radiologist productivity:
• Removed 3 radiologist slots from the schedule
• Developed Physician Accountability reports
• PowerScribe (increased self-edit rate; additional training; increased use of standardized templates)
• PACS (improved PACS default display protocols; improved ability to compare exams i.e. contracted hospital)
Additionally, the group was able to apply many other improvements that further streamlined the practice environment:
• Added reading stations to both hospital and imaging centers
• Up-trained MR techs for breast biopsies
• Improved layout of mammogram reading room
• Standardized tray for hospital US procedures
• Increased usage of IM for communication
• Increased the number of radiologists who perform common fluoroscopy procedures
• Improved connection speeds at various locations.
Results
In the end, the data the practice collects will provide the evidence the group needs to appreciate the impact of the interventions. By collecting and mapping the data throughout the process, the practice was able to demonstrate that it had indeed increased productivity and decreased variation.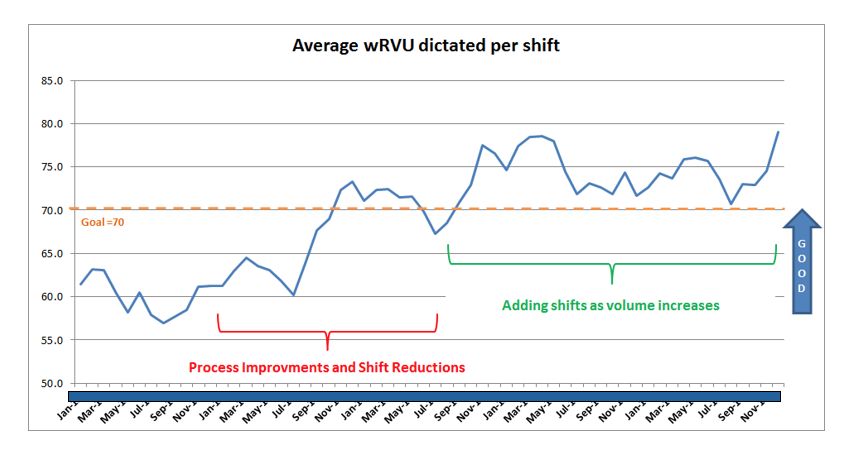
Radiology groups and departments interested in implementing lean methodologies in their practice setting will find ample resources to help them implement lean in the health care environment at the links identified below:
• CMS is an advocate for lean in health care
• Best practices are available at the Advisory Board Company
• Lean Enterprise Institute, an excellent source of education
• Gemba Academy – Video Training
• University of Michigan College of Engineering - Lean and Six Sigma healthcare courses and certifications
As you consider areas for improvement in your practice or the radiology department of your hospital, lean may be a method to utilize. If your hospital has a quality department or, better yet, a process improvement department with industrial engineers, contact them to propose some processes that are ready to be improved.
Lisa Mead, RN, MS, CPHQ, CHPC, is executive director, Strategic Radiology–Patient Safety Organization and a national consultant on quality improvement in health care.
Hub is the monthly newsletter published for the membership of Strategic Radiology practices. It includes coalition and practice news as well as news and commentary of interest to radiology professionals.
If you want to know more about Strategic Radiology, you are invited to subscribe to our monthly newsletter. Your email will not be shared.